The fifty-third anniversary of the Medicaid program on July 30 is an occasion to celebrate its accomplishments as well as contemplate ways to build on them. One way to do the latter would be to close the so-called Medicaid gap, so that the program could better fulfill its mission: to provide “medical assistance to individuals whose income and resources are insufficient to meet the costs of necessary medical services.”1
The Medicaid gap is a glaring inequity in our nation’s coverage system. More than 2 million uninsured adults currently have too much income to qualify for Medicaid in their states, but too little to qualify for tax credits for Health Insurance Marketplace plans’ premiums.2 Thirty-three states plus the District of Columbia have acted to close this gap by implementing Medicaid expansion under the Affordable Care Act (ACA); seventeen states, however, have not done so, leaving many of their residents stuck without affordable coverage.3
This gap persists, despite unprecedented federal financial support for Medicaid expansion. States would only have to pay, at most, 10 percent of total costs of this coverage—an amount that may be less than what states already pay for programs for the uninsured.4 Furthermore, rejecting program expansion is more than just a budgetary problem: significant evidence shows that people in the coverage gap get less needed health care, have greater medical bill debt, and have worse health outcomes.5
This report explores federal legislative pathways to accelerate the closing of the Medicaid gap, since such efforts have largely stalled in the wake of the 2012 Supreme Court decision on the ACA. All of these proposals could be free standing or complement broader public plan proposals currently being debated.
Background
Congress did not intentionally create the gap in Medicaid eligibility for certain low-income adults; it resulted from a Supreme Court decision. The ACA, as signed into law, created a seamless system of affordable health insurance coverage for Americans.6 Under this plan, Medicaid would, starting in 2014, expand to provide coverage for otherwise ineligible non-elderly adults in households with income below 138 percent of poverty, roughly the same Medicaid income eligibility level already available for young children. Above this nationwide floor, the ACA would provide people who otherwise lack access to affordable coverage with income-based premium tax credits for Health Insurance Marketplace plans.
The Medicaid expansion was drafted as a “mandatory eligibility group.” Since its start in 1965, the program has covered some groups of people who must be covered in order for a state to qualify for federal funding and others whose coverage is at state option. Unlike any previous mandatory or optional expansion, the ACA offers a high federal matching rate for the costs of this group: 100 percent from 2014 to 2016, phasing down to 90 percent by 2020.
However, in National Federation of Independent Businesses v. Sebelius (NFIB)7—the same case in which the Supreme Court upheld the constitutionality of the law’s individual mandate—a plurality of justices ruled that the mandatory Medicaid expansion provision of the ACA was unconstitutional. In a confusing opinion that had no precedent, the plurality found, first, that the newest mandatory expansion group, unlike many that had preceded it over the decades, amounted to a “shift in kind, not merely degree.” In other words, they concluded—over Justice Ruth Bader Ginsburg’s vigorous dissent—that the Medicaid expansion was not an extension of the traditional Medicaid program, but rather a new program. As such, the requirement to cover the Medicaid expansion population was a threat to terminate “other significant independent grants.”
The plurality then looked at whether that threat rose to the level of coercion, and found that the shift amounted to “economic dragooning,” analogous to the types of situations that the Court in the past had overturned under the Tenth Amendment.8 The plurality fashioned a remedy that, rather than overturning the expansion and its associated funding, barred the secretary of Health and Human Services from enforcing the expansion as a mandatory condition of Medicaid participation. In effect, the Court itself transformed the expansion—from a requirement to an option.
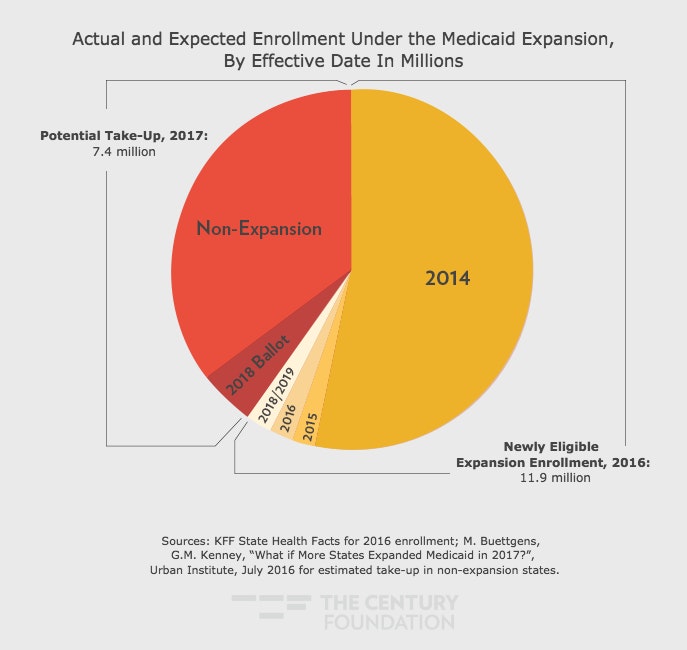
In the aftermath of this decision, over half of states implemented the Medicaid expansion in 2014, with three more in 2015 and two more in 2016. Maine’s expansion was set to start on July 1, 2018 but has been delayed in a legal battle.9 Virginia’s expansion will start on January 1, 2019. Three additional states—Idaho, Nebraska, and Utah—will likely have the Medicaid expansion on their ballots this November.10 In 2016, 12 million people were enrolled as newly eligible through the expansion (see Figure 1).11
Figure 1
In the states that have not implemented the Medicaid expansion, low-income adults are only eligible for Medicaid if they have a disability that meets Supplemental Security Income standards, are pregnant, or qualify for the mandatory eligibility category of adults with dependent children that is a vestige of when Medicaid was linked to welfare (unless the state has a Section 1115 demonstration waiver to cover childless adults, which only Wisconsin does). As of January 2018, the median eligibility limit for parents was 43 percent of the federal poverty level. The reasons offered for not implementing the expansion range from concern about cost to ideological opposition:12 every non-expansion state has a Republican governor, except North Carolina, which has a super-majority of Republicans in its state legislature.
This landscape has led to considerable research on the impact of the Medicaid expansion, as summarized in a recent literature review.13 The clearest effect is greater reductions in the uninsured rate in states that expanded Medicaid than in those that did not. This reduction in the uninsured has contributed to improved access to care, as found in dozens of studies. For example, low-income adults in expansion states reported a greater increase (12.1 percentage points) in having a personal physician and a greater reduction in cost-related barriers to care (18.2 percentage points) compared to those in a non-expansion state.14 The Medicaid expansion has also helped pay for treatment for people with behavioral health problems, including opioid addiction.15 These gains in access to care have translated into improved health outcomes (for example, lower mortality rates).16 The expansion also led to lower out-of-pocket costs for patients. One study found that the amount of debt sent to collection was reduced by over $1,000 per person in states that expanded Medicaid compared to those that did not expand the program.17 A recent study found no significant increase in state Medicaid spending, nor a decrease in education, transportation, or other state spending, as a result of the expansion.18 Health care providers, especially small, rural hospitals,19 have also gained financially from the Medicaid expansion.
Federal Pathways Forward to Expand Medicaid
To date, policy makers’ strategy to help those Americans caught in the Medicaid gap has been to urge states to implement the expansion. Support for the expansion has been an issue in gubernatorial elections such as that of Ralph Northam (D) in Virginia.20 As previously described, it also has become a ballot initiative in some states. This state-based approach has contributed to a number of Republican governors becoming champions for the expansion. For example, Ohio governor John Kasich has embraced it on economic and moral grounds.21 Such governors defended the ACA against attempts by the Republican-led White House and Congress to repeal and replace the ACA.22 Yet, under the status quo, it may take years if not decades for all states to embrace the ACA’s Medicaid expansion, leaving residents in these states at risk of worse health and financial insecurity.
Congress could change policy to accelerate the closing of the Medicaid gap. While the NFIB decision left a range of open questions, it does not prevent Congress from making legislative changes to further encourage implementation of the ACA’s Medicaid expansion. Below, we lay out a range of conceptual options. We believe that all six options presented fall within the bounds of the decision in NFIB, although expansion opponents would likely attempt to challenge some of these options, if enacted. Enactment of any one of these options would face political obstacles, including opposition due to the potential for increased costs. All of them would increase federal spending to the degree that they expand coverage (although quantifying these effects is beyond the scope of this report). This list of options does not include proposals to create entirely new programs, or to extend non-Medicaid assistance such as the Marketplaces’ premium tax credits to this group; rather, they strive to provide the expansion-eligible adult group with the same coverage as other Medicaid enrollees. Additional work would be needed to flesh these options out to ensure their effectiveness, efficiency, feasibility, and legality. They are presented in the order of those that would encounter the least challenges to their adoption to the most, in our estimation.
1. Increasing Federal Funding for the Medicaid Expansion
A straightforward approach to encouraging the remaining states to expand Medicaid is to increase federal financial support for doing so. In his fiscal year 2017 budget, President Obama proposed to provide states that newly expand Medicaid the same higher federal matching rate and six-year phase-down as those that expanded in 2014 (the ACA linked the federal financing to calendar years, assuming all states would implement the expansion in 2014).23 Senators Warner and Kaine (both D-VA) introduced this proposal, called the SAME Act (S. 1545).24 The Congressional Budget Office (CBO) projected that this policy would cost $31 billion over ten years.25 Congress could also vary increased federal financial incentives, such as extending the number of years that a newly expanding state gets 100 percent federal funding, or increasing the federal matching rate for such states from 90 percent to 95 percent, for example, for some extended length of time or in perpetuity.
Because the U.S. Supreme Court already upheld the ability of Congress to provide states with voluntary Medicaid expansion funds, nothing in NFIB would prevent Congress from “sweetening the deal” further. However, states such as Texas would probably not be swayed by even more generous federal financing for the expansion. Providing only newly expanding states with higher federal financing would also raise questions of equity among states that already implemented the expansion. While such legislation could offer all states higher federal matching payments than the ACA, including those states that already expanded would raise federal costs without increasing coverage in those states. Lastly, states may express skepticism that Congress would maintain that high level of federal support over time.
2. Linking New Program’s Funding to Medicaid Expansion
A second approach to encourage Medicaid expansion would be to set the terms for new health funding based, in part, on a state’s decision on whether to implement the Medicaid expansion. Specifically, the state matching rate for federal funds for a new health care program (for example, a block grant for opioid addiction treatment) would be higher for states that have not expanded Medicaid compared to those that have done so. For example, non-expansion states could pay the percent of costs that they do for most Medicaid spending, while expansion states could pay the same (lower) rate as they do for the Children’s Health Insurance Program (see Table 1). The allocation of the new federal funding under this approach would be blind to the Medicaid expansion; only the state contribution would be contingent on expansion.
Table 1
| State Share of Spending in Medicaid and the Children’s Health Insurance Program (CHIP), 2019 | ||
| Medicaid | CHIP | |
| Alabama | 28.1% | 0.0% |
| Alaska | 50.0% | 12.0% |
| Arizona | 30.2% | 0.0% |
| Arkansas | 29.5% | 0.0% |
| California | 50.0% | 12.0% |
| Colorado | 50.0% | 12.0% |
| Connecticut | 50.0% | 12.0% |
| Delaware | 42.5% | 6.7% |
| District of Columbia | 30.0% | 0.0% |
| Florida | 39.1% | 4.4% |
| Georgia | 32.4% | 0.0% |
| Hawaii | 46.1% | 9.3% |
| Idaho | 28.9% | 0.0% |
| Illinois | 49.7% | 11.8% |
| Indiana | 34.0% | 0.8% |
| Iowa | 40.1% | 5.1% |
| Kansas | 42.9% | 7.0% |
| Kentucky | 28.3% | 0.0% |
| Louisiana | 35.0% | 1.5% |
| Maine | 35.5% | 1.8% |
| Maryland | 50.0% | 12.0% |
| Massachusetts | 50.0% | 12.0% |
| Michigan | 35.6% | 1.9% |
| Minnesota | 50.0% | 12.0% |
| Mississippi | 23.6% | 0.0% |
| Missouri | 34.6% | 1.2% |
| Montana | 34.5% | 1.1% |
| Nebraska | 47.4% | 10.2% |
| Nevada | 35.1% | 1.6% |
| New Hampshire | 50.0% | 12.0% |
| New Jersey | 50.0% | 12.0% |
| New Mexico | 27.7% | 0.0% |
| New York | 50.0% | 12.0% |
| North Carolina | 32.8% | 0.0% |
| North Dakota | 50.0% | 12.0% |
| Ohio | 36.9% | 2.8% |
| Oklahoma | 37.6% | 3.3% |
| Oregon | 37.4% | 3.2% |
| Pennsylvania | 47.8% | 10.4% |
| Rhode Island | 47.4% | 10.2% |
| South Carolina | 28.8% | 0.0% |
| South Dakota | 43.3% | 7.3% |
| Tennessee | 34.1% | 0.9% |
| Texas | 41.8% | 6.3% |
| Utah | 30.3% | 0.0% |
| Vermont | 46.1% | 9.3% |
| Virginia | 50.0% | 12.0% |
| Washington | 50.0% | 12.0% |
| West Virginia | 25.7% | 0.0% |
| Wisconsin | 40.6% | 5.4% |
| Wyoming | 50.0% | 12.0% |
|
Note: 100% minus Federal Medical Assistance Percentages (FMAPs) for Medicaid and CHIP for fiscal year 2019. Source: Centers for Medicaid and Medicare Services. |
||
This approach would prevent new federal grant funding from being used to substitute for state and federal Medicaid expansion dollars. As experts suggested during the 2017 ACA debate, replacing behavioral health services provided by the Medicaid expansion with a state block grant will harm people with addiction by limiting access to Medicaid’s comprehensive care.26 Additionally, this approach would allow new funding to be targeted toward capacity expansion, supplemental services, or other complements to—rather than substitutes for—coverage. Programs such as the Ryan White HIV/AIDS Program have redefined their mission to complement Medicaid and other coverage programs to ensure support services along a continuum of care, adequate supply, and additional financial support for low-income people.27 This option also would promote a more level playing field financially: while non-expansion states may pay more for the new funds, they are paying less for Medicaid due to their decision not to expand.
The structure of this option avoids the core constitutional challenges present in NFIB, and while some opponents may attempt to question the germaneness of this condition (expanding Medicaid) to the new federal funding, the U.S. Supreme Court’s historical determinations around whether a condition has an underlying related policy goal—and thus is an appropriate use of Congress’ Spending Clause power—is quite broad.28 Moreover, this design has the added benefit of saving the federal government money on the new program, a feature that the Court has viewed favorably.29
This approach would allow state elected officials to argue that the expansion is an investment needed to gain additional federal funding at a lower state costs for popular initiatives. But, unless the new program was sizable, this incentive may be weak. A state may pay less for the higher matching rate for the new funds than it would to expand Medicaid. Poor states may additionally argue that they have the greatest need for the new program’s funding, yet have to pay more for the federal dollars than “rich” states to get it; some may decline participation altogether.
3. Allowing Cities or Counties to Expand Medicaid
Another option to expand Medicaid would be to bypass state governors and legislatures, instead allowing local jurisdictions to implement the Medicaid expansion within their borders. To take this option, local towns, cities, or counties would need to secure what would have otherwise been their state’s share of the total costs of the expansion of Medicaid in their jurisdictions. They would also need to work with the Centers for Medicare and Medicaid Services (CMS) to set up eligibility systems for their areas, using the HealthCare.gov website. Several of the same states targeted for Medicaid expansion already allow HealthCare.gov to determine Medicaid as well as Marketplace eligibility for people applying for health care coverage through the website. CMS also already reviews Medicaid managed care rates for currently eligible people in most of these states; it could use this information to leverage these rates for coverage for the city or county’s adult population. CMS would adopt benefits consistent with those offered to similarly situated Medicaid enrollees in the state, within the ACA’s guidelines for alternative benefit plans. The proposal would provide to this federally run Medicaid program the same rebates for prescription drugs that state-run Medicaid programs receive.
This proposal could cover many of the uninsured people in the Medicaid gap, if not most. Already, a number of municipalities conduct their own outreach efforts and have expressed support for the expansion. Roughly one million people would be covered through the Medicaid expansion if just six counties with a history of support for coverage expanded: Dallas, Harris (Houston), Miami-Dade, Hillsborough (Tampa), Fulton (Atlanta), and Salt Lake. It could also catalyze a subsequent state decision to expand Medicaid, since the cost to the state of covering eligible people in the rest of the state would be lower if the city or county funding continues.30 This route, like the first, avoids roadblocks created by NFIB, since states would not be required to do anything more than provide the same information to CMS that they already do.
That said, this option would undermine the concept of statewideness that has led to spillover gains in corners of states where low-income people have limited representation. It would also lead to confusion and perceived inequities within states. People in the suburbs of cities expanding Medicaid would be ineligible. Rural areas typically lack the tax base to support initiatives such as this. This proposal could further exacerbate disparities between areas based on wealth, population density, and politics, since Democratic policy makers (more likely to hold office in large urban areas) have been more inclined to expand Medicaid. Within local areas that expand, there would also need to be protocols for adults whose income fluctuates and thus shifts their eligibility between state and local Medicaid programs. It is possible that, under this policy, there may be additional political fights in ardently anti-ACA states if opponents push for particularly mean-spirited state preemption policies—in other words, if state officials try and pass legislation prohibiting localities from pursuing these options, which may or may not run into state legal roadblocks.
4. Making Medicaid Adult Coverage “All or Nothing” for States
A fourth proposal for expanding Medicaid is less about financing than control over coverage, and is modeled on the legislation passed to create the Medicare drug benefit. It would give states a choice: cover all low-income adults, or none. If they decline, then the federal government would assume responsibility for covering non-disabled, non-elderly adults in both pre-ACA and the ACA expansion eligibility groups. A state not implementing the Medicaid expansion would no longer receive federal matching payments for adults with dependent children (and potentially related groups). Instead, CMS would operate a federal Medicaid program for those adults. Since all non-expansion states use HealthCare.gov for eligibility determinations for premium tax credits, CMS would use this system for eligibility determinations for this Medicaid-like program. The program’s benefits would be determined as previously described for the option in which federal Medicaid is offered in cities and counties. Enrollees would also have the same rights as Medicaid enrollees (for example, to a timely appeal of an eligibility determination).
This proposal would be similar to the approach taken when Medicare created a drug benefit that states had previously provided to low-income seniors. As they do for the Medicare Part D drug benefit, states that decline to expand would be required to make a “clawback” payment to the federal government, estimated to be equal to their previous spending on relevant adults with dependent children (adjusted for trends). Additionally, CMS would collect fees (potentially through Medicare) from insurance coverage providers and plans in that state to finance what would have been the state share of the expansion. Providers’ taxes are already a common source of state funding for the Medicaid expansion.31 This option’s funding approach aims to prevent a state that has already expanded Medicaid from achieving savings from shifting its enrollees into the federally run Medicaid program; it would also charge a fee to such a state for the cost of the transition, in part to ensure seamless coverage.
If CMS ran just the Medicaid expansion as a federal program, it would legally be no different than its operation of Medicare. But, because this option transfers both the coverage of and state funding for currently Medicaid-eligible adults to the federal Medicaid program, it might trigger a coercion analysis under NFIB. However, opponents would face a difficult task to show that the threat of lost funds, when replaced through equivalent federal dollars put back into expanding coverage in the state and into the state economy, would constitute “economic dragooning.” States would lose a share of federal Medicaid spending (roughly 6 percent in Texas, for example, and up to 15 percent in Florida32), but there would be no political or economic “gun to the head” when people obtained the same coverage funded from another source.
The rationale for this option is that states may prefer to keep control over coverage of this group rather than cede it to the federal government. Additionally, uniquely under this option, states could not block expansion: their choice, instead, would be whether or not to run the expansion along with coverage for adults already eligible for Medicaid. It is unclear to the authors of this report which option states would take. States have increasingly applied work requirements, premiums, and other complex eligibility requirements to low-income adults in Medicaid; states may prefer to give up management of coverage for this group altogether. This proposal would also result in a disconnect in coverage for parents in federally run Medicaid and children in state-run Medicaid. Should states that already expanded Medicaid prefer this option, it would increase the implementation challenge and complexity of the system.
5. Leveraging Federal Hospital Funding for Medicaid Expansion
A more aggressive policy option would be to redirect existing federal spending rather than new federal funding in response to a state’s lack of a Medicaid expansion. This option could take the form of changes to Medicaid’s disproportionate share hospital (DSH) payment program. Created to support hospitals that disproportionately care for Medicaid enrollees and uninsured patients, the optional DSH program has come under increasing federal oversight since the 1990s. In part, this results from evidence that states have not targeted DSH spending toward its original purpose; for example, in 2012, about one-third of DSH payments were made to hospitals that did not meet program standards.
Under this option, Congress would replace federal Medicaid DSH allotments with a new, fully federal, highly targeted payment program for hospitals in such states—without reducing federal funding for these states’ hospitals. Congress would set a funding formula for these states’ hospitals based on uninsured patients’ costs, and pay them via the Medicare program (for example, as an add-on to Medicare’s own DSH payment program which serves a similar, although not identical, purpose). Federal DSH allotments and states’ uses of them would remain unchanged for states that have expanded Medicaid. States that want to maintain control of federal DSH allotments would have an incentive to expand Medicaid.
The rationale is that expansion states have lowered their hospital uncompensated care, and thus are best positioned to allocate federal DSH funds for Medicaid payment shortfalls and related purposes. Yet, other states’ decisions to forgo Medicaid expansion results in significantly greater uncompensated care for more uninsured patients. As such, a congressionally set formula to allocate federal Medicaid DSH allotments to hospitals with the greatest uncompensated care burdens in such states would better fulfill the program’s purpose than non-expansion states’ current allocation formulas. Non-expansion states would be free to use their current state spending for DSH payments to pay hospitals in any way that they prefer, including to compensate hospitals for low Medicaid payment rates. But they would no longer be able to draw down federal funding for a broad set of uses. A state interested in maintaining its current federal-state DSH program could do so by expanding Medicaid.
In nine of the seventeen states that have not expanded Medicaid, the projected loss of control over federal DSH funding for fiscal year 2019 exceeds the projected state spending to fully implement the Medicaid expansion (see Table 2). Even where the state expansion costs exceed potential lost control over federal DSH funding, state policy makers may place a nonmonetary value on their ability to allocate federal DSH funding. Historically, states used federal DSH payments to return to hospitals some of the taxes they pay to offset state costs; while federal rules prevent egregious kick-back schemes, this proposal could upset the balance in financing Medicaid in some states. Hospitals would be held harmless in aggregate at the state level, but each hospital would likely get a different amount based on a statutory formula than what the state-based formula offered. As such, this proposal would likely be opposed by some hospitals and states on the grounds that it upsets long-standing arrangements that support local provision of health care to low-income people. Conversely, some hospitals would prefer such a national approach. Some states have invested little in DSH and thus this proposal would not alter their calculus.
Table 2
| Comparison of Estimated State Costs for Medicaid Expansion and Federal Disproportionate Share Hospital (DSH) Allotments, 2019 | |||
| Non-Expansion State | Estimated State Cost of Expansion | Federal DSH Allotments | Difference |
| Alabama | $97,000,000 | $353,600,000 | ($256,600,000) |
| Florida | $187,000,000 | $230,000,000 | ($43,000,000) |
| Georgia | $246,000,000 | $309,100,000 | ($63,100,000) |
| Idaho | $39,000,000 | $18,900,000 | $20,100,000 |
| Kansas | $58,000,000 | $47,400,000 | $10,600,000 |
| Mississippi | $93,000,000 | $175,400,000 | ($82,400,000) |
| Missouri | $101,000,000 | $544,800,000 | ($443,800,000) |
| Nebraska | $36,000,000 | $32,500,000 | $3,500,000 |
| North Carolina | $112,000,000 | $339,300,000 | ($227,300,000) |
| Oklahoma | $117,000,000 | $41,600,000 | $75,400,000 |
| South Carolina | $111,000,000 | $376,600,000 | ($265,600,000) |
| South Dakota | $22,000,000 | $12,700,000 | $9,300,000 |
| Tennessee | $191,000,000 | $53,100,000 | $137,900,000 |
| Texas | $984,000,000 | $1,099,700,000 | ($115,700,000) |
| Utah | $67,000,000 | $22,600,000 | $44,400,000 |
| Wisconsin | ($107,000,000) | $108,700,000 | ($215,700,000) |
| Wyoming | $15,000,000 | $300,000 | $14,700,000 |
| Total | $2,369,000,000 | $3,766,300,000 | ($1,397,300,000) |
|
Note: For fiscal year 2019. Sources: M. Buettgens, “Implications of Medicaid Expansion in the Remaining States: 2018 Update,” Urban Institute, May 2018; MACPAC, Report to Congress on Medicaid and CHIP, March 2018. |
|||
Despite the restrictions that NFIB placed on adding separate conditions on existing, independent programs, the plurality in the Court’s decision does not completely cut off that option if a condition does not reach the level of a “gun to the head.”33 One such example of a non-coercive condition attached to a program was the loss of some highway funds that were less than 1 percent of state budgets, a loss that would at most be a small percentage of the overall highway funding provided to states.34 A loss of state control over DSH payments—that are subsequently replaced with federal payments that address the same problem—would not impact the overall state fiscal situation in the same way a state budget cut without that replacement might. In fact, the overall federal dollars flowing into a state’s economy would be the same. And the impact on the state’s overall budget would likely fall within a range deemed non-coercive by the Court, as federal DSH payments to state would generally fall below 1 percent of overall state budgets ($12 billion in federal DSH,35 compared to nearly $2 trillion in state budgets36 in 2017). That said, this approach may be legally, as well as politically, fraught.
6. Penalizing Non-Expansion States
Lastly, policy makers could develop legislation for a straightforward choice between Medicaid expansion or a modest penalty for states, in the form of a reduction of one to two percentage points (maybe up to five points) in the federal matching rate for Medicaid in states that do not implement the expansion. The penalty amount would be set to be meaningful but not coercive, and like the condition attached to highway funds, it would be around 1 percent of state budgets (less than $2 billion in states that have not expanded Medicaid37)—far lower than the penalty written into the ACA. Such an approach was adopted by Congress in the early 1970s to sanction states that failed to actively implement Medicaid’s early and periodic screening, diagnosis, and treatment benefits (EPSDT) for children. Such states would lose 1 percent of the federal share of their grants for Aids to Families with Dependent Children (AFDC). The amount could be calibrated. The rationale for this policy is that their failure to expand Medicaid increases federal uncompensated care payments via Medicare’s DSH program, shifting costs to the federal budget.
In the post-NFIB world, opponents may cry “coercion” even for a modest penalty approach, especially when attached to an eligibility group considered a “shift in kind, not degree”—that is, a non-traditional group. However, a reasonable interpretation of NFIB leaves room for the existence of a related condition that would not reach the level of unconstitutional “economic dragooning.” This type of approach also inevitably would face severe political and policy constraints as well, since states would claim that the penalty ultimately falls on impoverished people residing in states already considered to be the least generous toward their poorest populations. This is essentially why the EPSDT penalty never was imposed.
Discussion
These proposals go beyond the current generous federal financing to fill the Medicaid gap. Each of them targets a different barrier and thus their efficacy would vary. For example, if the state opposition to expansion reflects anti-government sentiments, then the proposal to allow interested local officials circumvent this opposition might best reduce coverage disparities within such states. If, instead, the state officials have a bias toward the status quo, they may prefer to expand Medicaid than lose control over federal funding for their state-designed DSH program. In states with a narrow political margin, supporters could use either a more generous federal matching rate for expansion or lower state costs of new grant funding as leverage to induce them to fill their gap. Only the fourth option— “all or nothing” —would ensure coverage in the gap irrespective of state decisions.
The options also implicate NFIB to varying degrees. Some simply avoid the constitutional questions created by the original expansion—and subsequent limitations delineated by the Court—by expanding the role of the federal government or localities and bypassing states. Others make a reasonable assessment of the boundaries of the NFIB decision and design incentives to end state inaction that fall within those boundaries.
Putting aside their particular features, these proposals to fill the Medicaid gap would help alleviate arguably the most acute barrier to access to care left in our health system. They could supplement more comprehensive proposals—such as those that expand public plan options—that include all uninsured Americans but may lack tailored benefits or financial assistance for poor adults. Moreover, beyond Medicaid’s efficacy, the program is popular: 74 percent of Americans have a favorable view of it.38 That said, these options for filling the Medicaid gap will be considered partisan—if only because every non-expansion state is led by Republicans. As such, a Republican Congress would be unlikely to even allow such proposals to come up for a vote. However, this could change over time. Given the health disparities between residents in states that have and have not expanded Medicaid, these and similar proposals should be aggressively explored.
Acknowledgements
We thank Sara Rosenbaum, Michael Sparer, and Sylvia Law for sharing their extensive knowledge, insight, and suggestions on the Medicaid legal and policy landscape and these options and their considerations.
Notes
- Section 1901, Social Security Act.
- Rachel Garfield, Anthony Damico, and Kendal Orgera, “The Coverage Gap: Uninsured Poor Adults in States that Do Not Expand Medicaid,” Kaiser Family Foundation, June 2018, http://files.kff.org/attachment/Issue-The-Coverage-Gap-Uninsured-Poor-Adults-in-States-that-Do-Not-Expand-Medicaid.
- State Health Facts, “Status of State Action on the Medicaid Expansion Decision,” Kaiser Family Foundation, July 3, 2018, https://www.kff.org/health-reform/state-indicator/state-activity-around-expanding-medicaid-under-the-affordable-care-act/?currentTimeframe=0&sortModel=%7B%22colId%22:%22Location%22,%22sort%22:%22asc%22%7D.
- Jesse Cross-Call, “Medicaid Expansion Producing State Savings and Connecting Vulnerable Groups to Care,” Center on Budget and Policy Priorities, June 15, 2016, https://www.cbpp.org/research/health/medicaid-expansion-producing-state-savings-and-connecting-vulnerable-groups-to-care.
- Larisa Antonisse, Rachel Garfield, Robin Rudowitz, and Samantha Artiga, “The Effects of Medicaid Expansion under the ACA: Updated Findings from a Literature Review,” Kaiser Family Foundation, March 28, 2018, https://www.kff.org/medicaid/issue-brief/the-effects-of-medicaid-expansion-under-the-aca-updated-findings-from-a-literature-review-march-2018/.
- Individuals who are citizens, nationals, or lawfully present in the United States are eligible for Health Insurance Marketplace subsidies and coverage. Lawfully present immigrants are generally eligible for the Medicaid expansion after a five-year waiting period.
- National Federation of Independent Business v. Sebelius, 567 U.S. 519 (2012).
- The Court here conflates the need for conditions to be germane to the underlying policy and the restriction on a condition being overly coercive. Previously, the Court had focused primarily on whether a condition of spending was related to the underlying purpose, but had spent far less time analyzing the role that coercion might play in determining whether a condition is constitutional. The Court also considers, but does not seem to find dispositive, whether a state had adequate notice of the condition.
- Patty Wight, “Medicaid Expansion Battle Moves to Maine Supreme Court,” Maine Public, July 18, 2018, http://mainepublic.org/post/medicaid-expansion-battle-moves-maine-supreme-court#stream/0.
- Max Greenwood, “Medicaid Expansion Likely to Appear on November Ballot in Nebraska,” The Hill, July 5, 2018, http://thehill.com/homenews/state-watch/395703-medicaid-expansion-likely-to-appear-on-ballot-in-nebraska.
- State Health Facts, “Medicaid Expansion Enrollment, FY 2016,” Kaiser Family Foundation, accessed July 23, 2018, https://www.kff.org/health-reform/state-indicator/medicaid-expansion-enrollment/?currentTimeframe=0&sortModel=%7B%22colId%22:%22Location%22,%22sort%22:%22asc%22%7D.
- Amanda Woolfe, “Why Haven’t More States Expanded Medicaid?” California Healthline, June 25, 2014, https://californiahealthline.org/news/why-havent-more-states-expanded-medicaid-yet/.
- Larisa Antonisse, Rachel Garfield, Robin Rudowitz, and Samantha Artiga, “The Effects of Medicaid Expansion under the ACA: Updated Findings from a Literature Review,” Kaiser Family Foundation, March 28, 2018, https://www.kff.org/medicaid/issue-brief/the-effects-of-medicaid-expansion-under-the-aca-updated-findings-from-a-literature-review-march-2018/.
- Benjamim D. Sommers, Robert J. Blendon, John Orav, et al., “Changes in Utilization and Health Among Low-Income Adults After Medicaid Expansion or Expanded Private Insurance,” JAMA Internal Medicine 176, no. 1 (2016):1501–09, https://jamanetwork.com/journals/jamainternalmedicine/fullarticle/2542420.
- Lisa Clemens-Cope, Marni Epstein, and Genevieve M. Kenney, “Rapid Growth in Medicaid Spending on Medications to Treat Opioid Use Disorder and Overdose,” Urban Institute, 2017, http://www.urban.org/sites/default/files/publication/91521/2001386-rapid-growth-in-medicaid-spending-on-medications-to-treat-opioid-use-disorder-and-overdose_3.pdf.
- Benjamin D. Sommers, Katherine Baicker, and Arnold M. Epstein, “Mortality and Access to Care among Adults after State Medicaid Expansions,” New England Journal of Medicine, September 13, 2012, http://www.nejm.org/doi/full/10.1056/nejmsa1202099.
- Luojia Hu, Robert Kaestner, Bhashkar Mazumder, Sarah Miller, and Ashley Wong “The Effect of the Patient Protection and Affordable Care Act Medicaid Expansions on Financial Well-Being,” National Bureau of Economic Research, no. 22170, 2016, http://www.nber.org/papers/w22170.pdf.
- Benjamin D. Sommers and Jonathan Gruber, “Federal Funding Insulated State Budgets from Increased Spending Related to Medicaid Expansion,” Health Affairs 65, no. 5 (May 2017): 938–44, https://www.healthaffairs.org/doi/pdf/10.1377/hlthaff.2016.1666.
- Frederic Blavin, “How Has the ACA Changed Finances for Different Types of Hospitals? Updated Insights from 2015 Cost Report Data,” Urban Institute, April 2017, https://www.rwjf.org/content/dam/farm/reports/issue_briefs/2017/rwjf436310.
- Scott Clement and Emily Guskin, “Exit Poll Results: How Different Groups of Virginians Voted,” Washington Post, November 8, 2017, https://www.washingtonpost.com/graphics/2017/local/virginia-politics/governor-exit-polls/?utm_term=.55399c5c37e3.
- Dan Zak, “Spurning the Party Line,” Washington Post, January 5, 2016, https://www.washingtonpost.com/sf/national/2016/01/05/deciderskasich/?noredirect=on&utm_term=.bf98a47bfbea.
- Sean Sullivan, Juliet Eilperin, and Kelsey Snell, “New Health-Care Plan Stumbles under Opposition from Governors,” Washington Post, September 19, 2017, https://www.washingtonpost.com/powerpost/renewed-obamacare-repeal-effort-dealt-a-blow-as-governors-come-out-in-opposition/2017/09/19/499478fe-9d51-11e7-9083-fbfddf6804c2_story.html?utm_term=.34eb00bd6e6d.
- Office of Management and Budget, Budget of the U.S. Government, Fiscal Year 2017 (Washington, D.C.: U.S. Government Printing Office, 2016), https://obamawhitehouse.archives.gov/sites/default/files/omb/budget/fy2017/assets/budget.pdf.
- S.1545—SAME Act of 2017, 115th Congress (2017–18).
- Congressional Budget Office, “An Analysis of the President’s 2017 Budget,” March 2016, https://www.cbo.gov/sites/default/files/114th-congress-2015-2016/reports/51383-apb.pdf.
- Richard G. Frank, “Ending Medicaid Expansion Will Leave People Struggling with Addiction without Care,” The Hill, June 20, 2017, http://thehill.com/blogs/pundits-blog/healthcare/338579-ending-medicaid-expansion-will-leave-people-struggling-with.
- Sean R. Cahill, Kenneth H. Mayer, and Stephen L. Boswell, “The Ryan White HIV/AIDS Program in the Age of Health Reform,” American Journal of Public Health 105, no. 6 (June 2015): 1078–85, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4431102/.
- South Dakota v. Dole, 483 U.S. 203 (1987).
- National Federation of Independent Business v. Sebelius, 567 U.S. 519 (2012), citing Steward Machine Company v. Davis, 301 U.S. 548 (1937).
- This estimate is based on the Urban Institute estimate for the number of people covered by the expansion group (“What If More States Expanded Medicaid in 2017? Changes in Eligibility, Enrollment, and the Uninsured,” Urban Institute, July 2016, http://www.urban.org/sites/default/files/publication/82786/2000866-What-if-More-States-Expanded-Medicaid-in-2017-Changes-in-Eligibility-Enrollment-and-the-Uninsured.pdf) multiplied by these counties’ share of their state’s population in poverty (United States Census Bureau, 2017, https://www.census.gov/quickfacts/fact/table/US/PST045217).
- Adam Searing, “’Budget Neutral’ Funding for State Share of Medicaid Expansion: Hospital Fees and Taxes?” Georgetown University Health Policy Institute, Center for Children and Families, January 29, 2015, https://ccf.georgetown.edu/2015/01/29/budget-neutral-funding-state-share-medicaid-expansion-hospital-fees-taxes/.
- Calculated based on data in State Health Facts, Kaiser Family Foundation, https://www.kff.org/statedata/.
- National Federation of Independent Business v. Sebelius, 567 U.S. 519 (2012).
- South Dakota v. Dole, 483 U.S. 203 (1987).
- State Health Facts, “Federal Medicaid Disproportionate Share Hospital (DSH) Allotments, FY 2017,” Kaiser Family Foundation, https://www.kff.org/medicaid/state-indicator/federal-dsh-allotments/?currentTimeframe=0&sortModel=%7B%22colId%22:%22Location%22,%22sort%22:%22asc%22%7D.
- National Association of State Budget Officers, “Summary: NASBO State Expenditure Report,” NASBO, November 16, 2017, https://higherlogicdownload.s3.amazonaws.com/NASBO/9d2d2db1-c943-4f1b-b750-0fca152d64c2/UploadedImages/Issue%20Briefs%20/State_Expenditure_Report_Summary_FY15-17.pdf.
- Calculated based on State Health Facts, “Total State Expenditures, SFY 2016,” Kaiser Family Foundation, https://www.kff.org/other/state-indicator/total-state-spending/?currentTimeframe=0&sortModel=%7B%22colId%22:%22Location%22,%22sort%22:%22asc%22%7D.
- Ashley Kirzinger, Bryan Wu, and Mollyann Brodie, “Kaiser Health Tracking Poll—February 2018: Health Care and the 2018 Midterms, Attitudes Towards Proposed Changes to Medicaid,” Kaiser Family Foundation, March 1, 2018, https://www.kff.org/health-reform/poll-finding/kaiser-health-tracking-poll-february-2018-health-care-2018-midterms-proposed-changes-to-medicaid/.