The Affordable Care Act (ACA) was signed into law twelve years ago, on March 23, 2010. In the years since, the United States has seen remarkable progress in access to affordable health coverage and health care. Before the law was passed, around 18 percent of the population—more than 46.5 million people—were uninsured. The most recent estimates from mid-2021 put that number now at only 8.9 percent, or about 29.5 million people.
These gains in coverage were concentrated among marginalized groups who were more likely to lack health coverage before the ACA was enacted. Far too many Americans remain uninsured and underinsured, however. This commentary outlines how several provisions of the ACA improved health equity—ensuring that every person has a fair opportunity to be healthy regardless of their social circumstance or identities—for women, LGBTQ people, and people of color. It also describes several ways to build on the successes and structure of the ACA to move further toward universal health coverage, a necessary component of achieving full health equity.
Coverage Affordability
As the name suggests, several components of the Affordable Care Act focused on making health coverage more affordable for consumers who struggled to maintain care due to cost. In this section, we describe how two of these—Medicaid expansion and pre-existing conditions protections—have made health coverage much more affordable for women, LGBTQ people, and people of color.
Medicaid Expansion
Medicaid is a joint state and federal program that provides public health insurance to low-income households. States generally have leeway to set the eligibility and benefit standards for their residents, within broad federal guidelines. The ACA originally sought to require all states to cover every resident up to 138 percent of the federal poverty line (FPL), addressing the patchwork of thresholds that often left childless adults ineligible even at 0 percent of the FPL. Under this expansion, the federal government would pay 90 percent of the costs associated with the newly eligible population. While the requirement to expand Medicaid was eventually found unconstitutional, Medicaid expansion was kept in place as an option for states, and most states and the District of Columbia have expanded Medicaid under the law.
All three groups that this piece focuses on are more likely to have lower incomes. In 2019, women were more than 20 percent more likely than men to have incomes below the poverty line. Similarly, the poverty rate for Black people was more than 2.5 times higher than it was for white people in 2019, and it was more than twice as high for Hispanic people in the same year. Researchers at UCLA estimated in 2019 that LGBTQ people were around 37.5 percent more likely to have incomes below the poverty line as cisgender, heterosexual people. These major disparities in income resulted in Medicaid expansion under the ACA improving all three groups’ access to high quality, affordable coverage.
However, because Medicaid expansion eventually was made voluntary for states rather than a requirement, the efficacy of the provision was reduced. Around 2.2 million people fall into the Medicaid coverage gap—that is, their incomes are too high for their states’ non-expanded Medicaid program, but too low to afford another source of coverage. Eight of the twelve states that have not yet expanded Medicaid are in the South and have disproportionately high Black and Hispanic populations, meaning these states’ decision not to expand raises severe health equity concerns.
Medicaid expansion not only improved access to coverage, but also is associated with improvements in health outcomes. Medicaid coverage of pregnancy-related care is extremely generous, and it is provided with no cost-sharing to the pregnant person. As a result, states that expanded Medicaid have around 1.6 fewer maternal deaths per 100,000 women than states that have not. This is especially crucial to improving health equity, as Black women are roughly three times as likely to die from pregnancy-related causes as white women.
Pre-existing Conditions
In addition to Medicaid expansion, the ACA made several changes to how private health insurance operates. Prior to the law, health insurance companies could charge a higher premium or decline coverage outright based on a person’s medical history. In essence, health coverage was least affordable for the people who needed it most. To address this, the ACA prohibits health insurers from charging people different premiums for any reason beyond age, zip code, and smoking status.
Prohibiting discrimination based on pre-existing conditions has also likely had an outsized impact on women, LGBTQ people, and people of color. All three groups are more likely to have pre-existing conditions that would have precluded them from coverage (or made that coverage far more expensive) before the protections the ACA afforded, and when these identities intersect, it’s even more likely. Many insurers would keep a list of “declinable conditions,” and if a person reported one of these in their medical history, they would be automatically denied coverage.
For example, before the ACA, many health insurers would refuse to cover a pregnant person or would charge a higher premium to a person who had been pregnant before. HIV/AIDS was another condition that was often used to deny or limit coverage before the ACA. Men who have sex with men (MSM) have a one in six chance of contracting HIV in their lifetime, and for Black or Latino MSM, that risk rises to one in two and one in four, respectively. And because of systemic racism, people of color are more likely to have a chronic health condition: 13.8 percent of Black people and 10 percent of Hispanic people have a chronic health condition, compared to only 8.3 percent of white people. Without the protections of the ACA, all of these health conditions could have been used to deny coverage or charge higher premiums.
Coverage Gains under the ACA
The ACA has made health insurance more accessible—particularly for women, people of color, and LGBTQ people. Its provisions, especially Medicaid expansion, have made insurance more affordable and have resulted in substantial gains in health coverage.
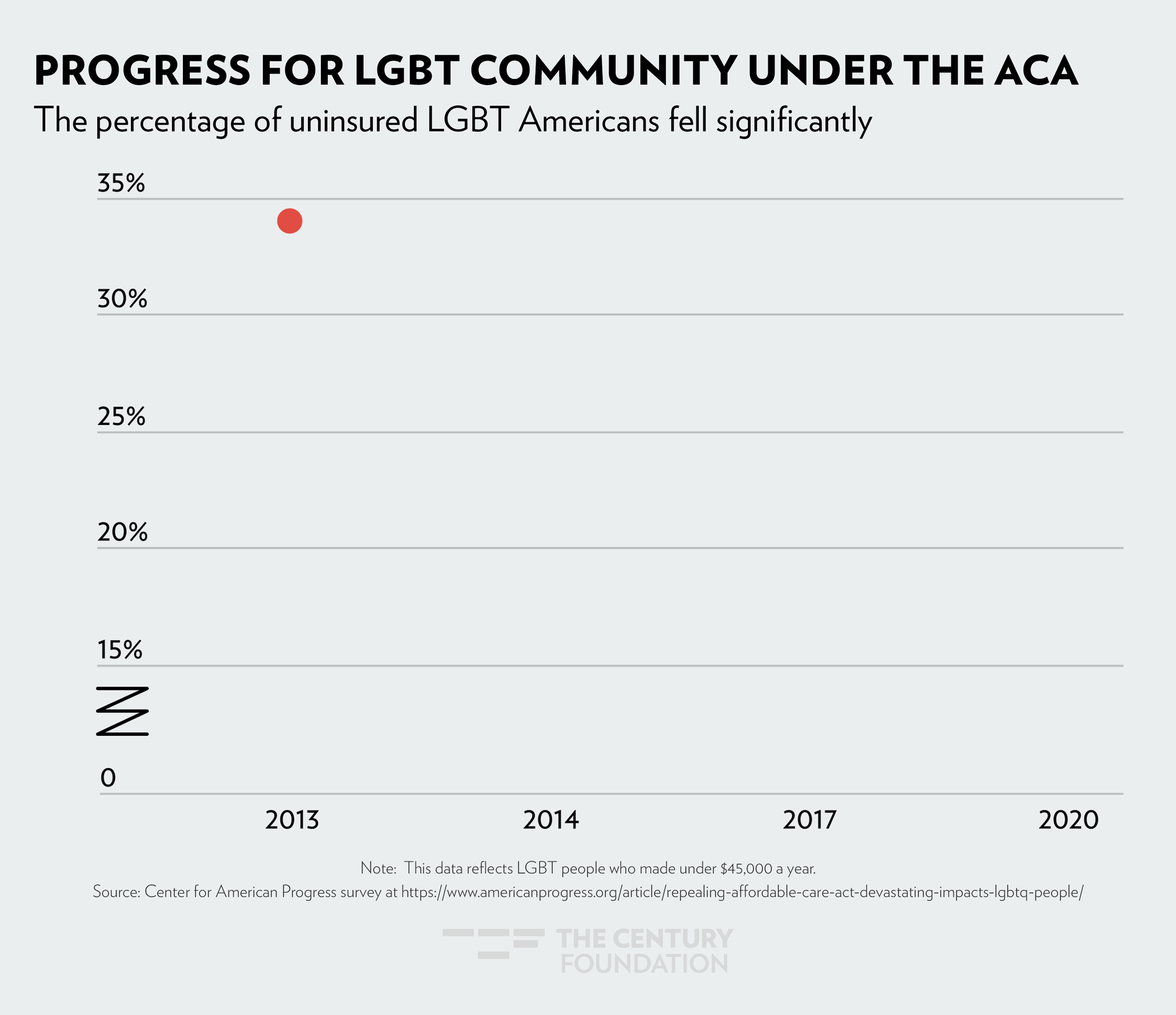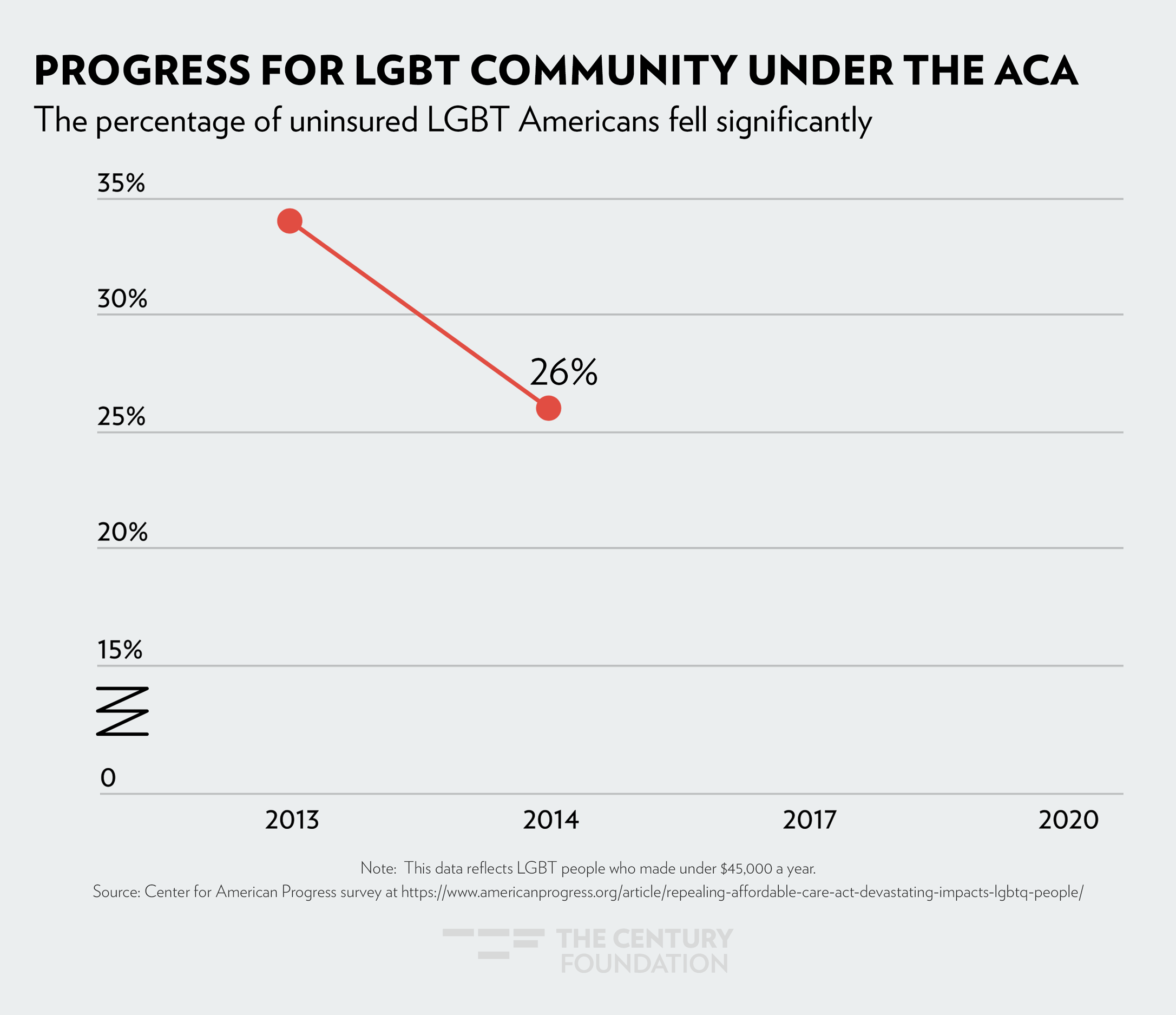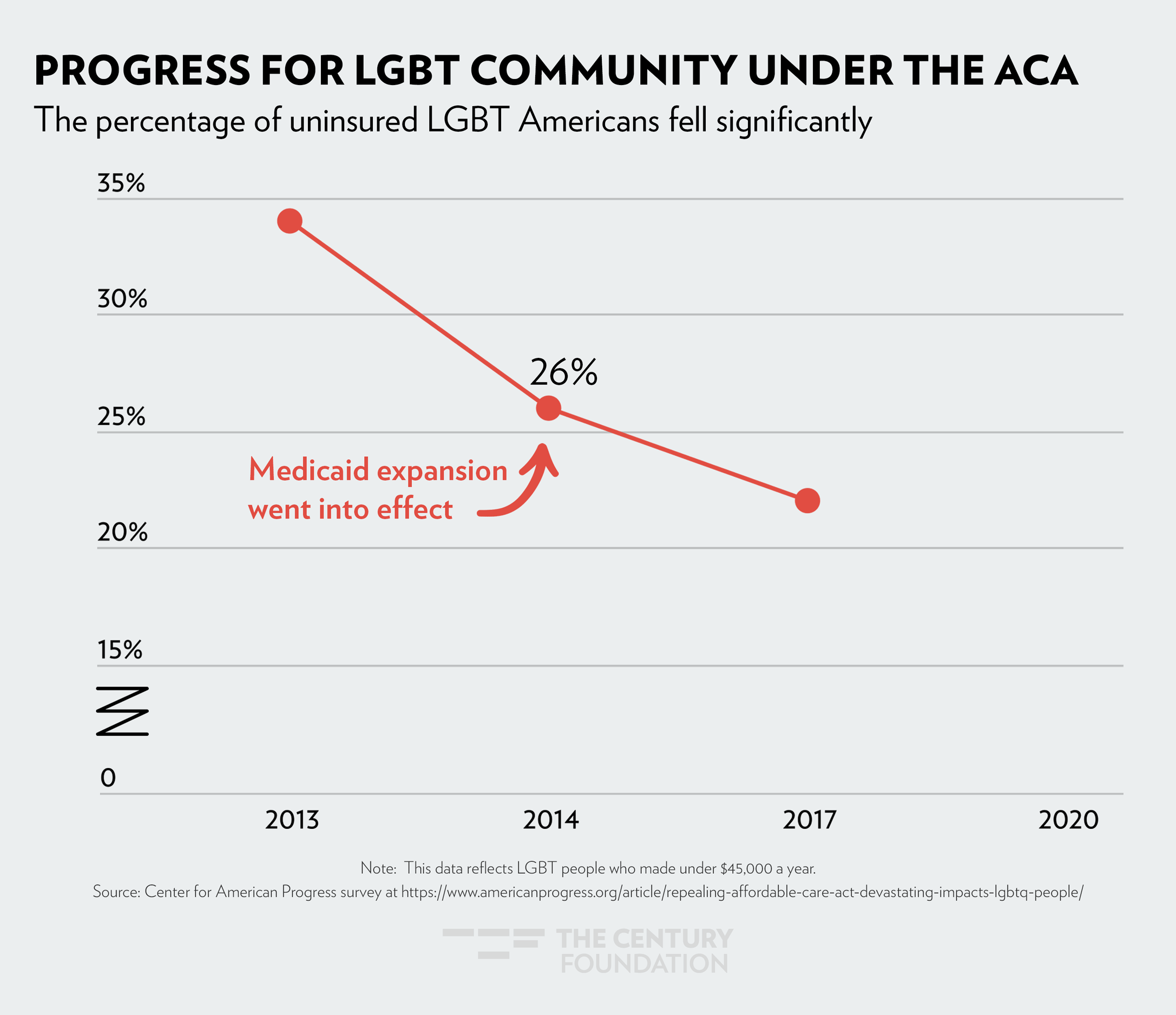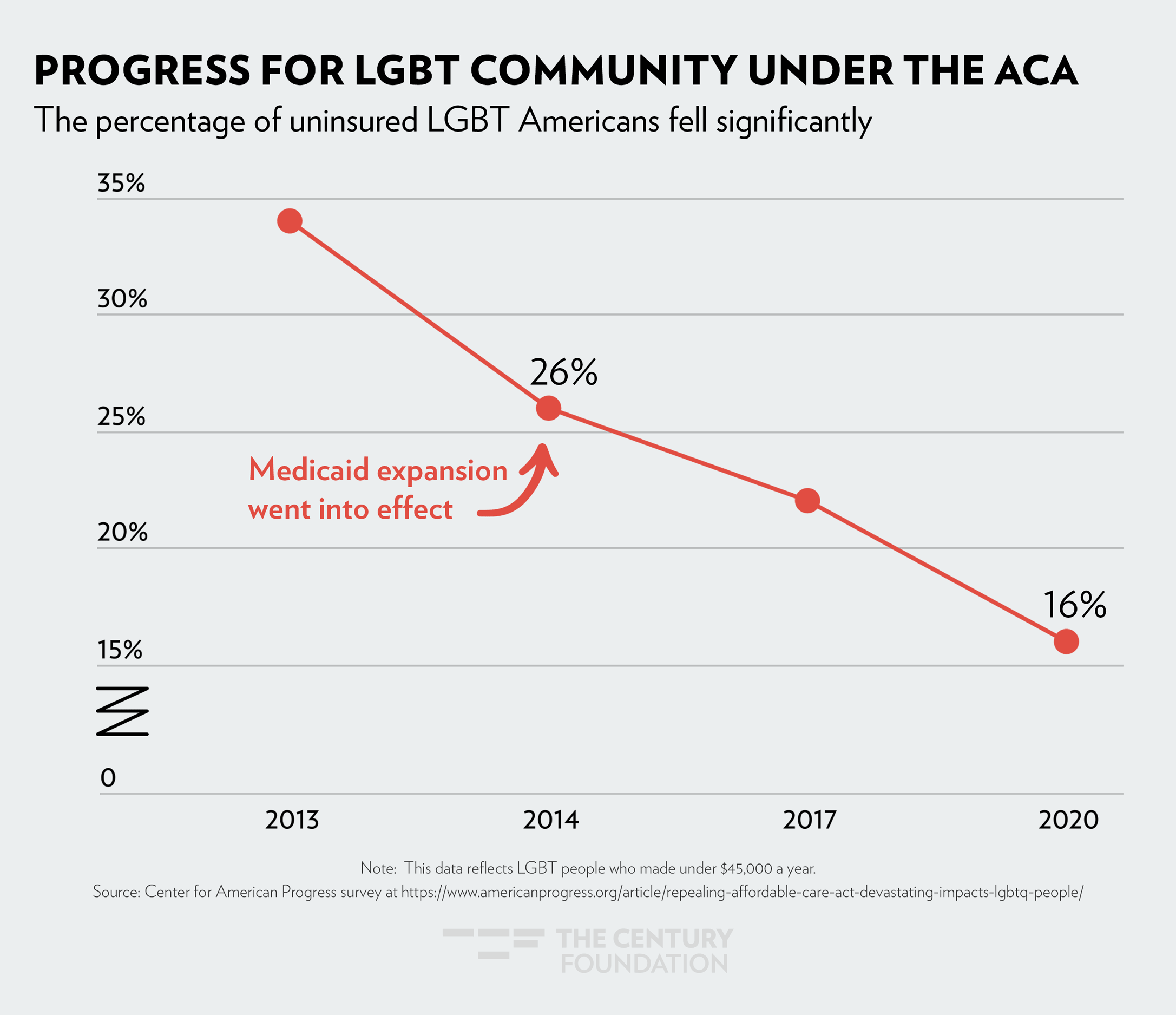
The sharpest drop in health coverage was seen in 2014, when Medicaid expansion went into effect. The figures below demonstrate the impact Medicaid expansion has had, by community: Figure 1 shows the decrease in women’s uninsured rate since 2010; Figure 2 shows health coverage by race and ethnicity; and Figure 3 shows how LGBTQ people have gained coverage under the ACA.
Figure 1
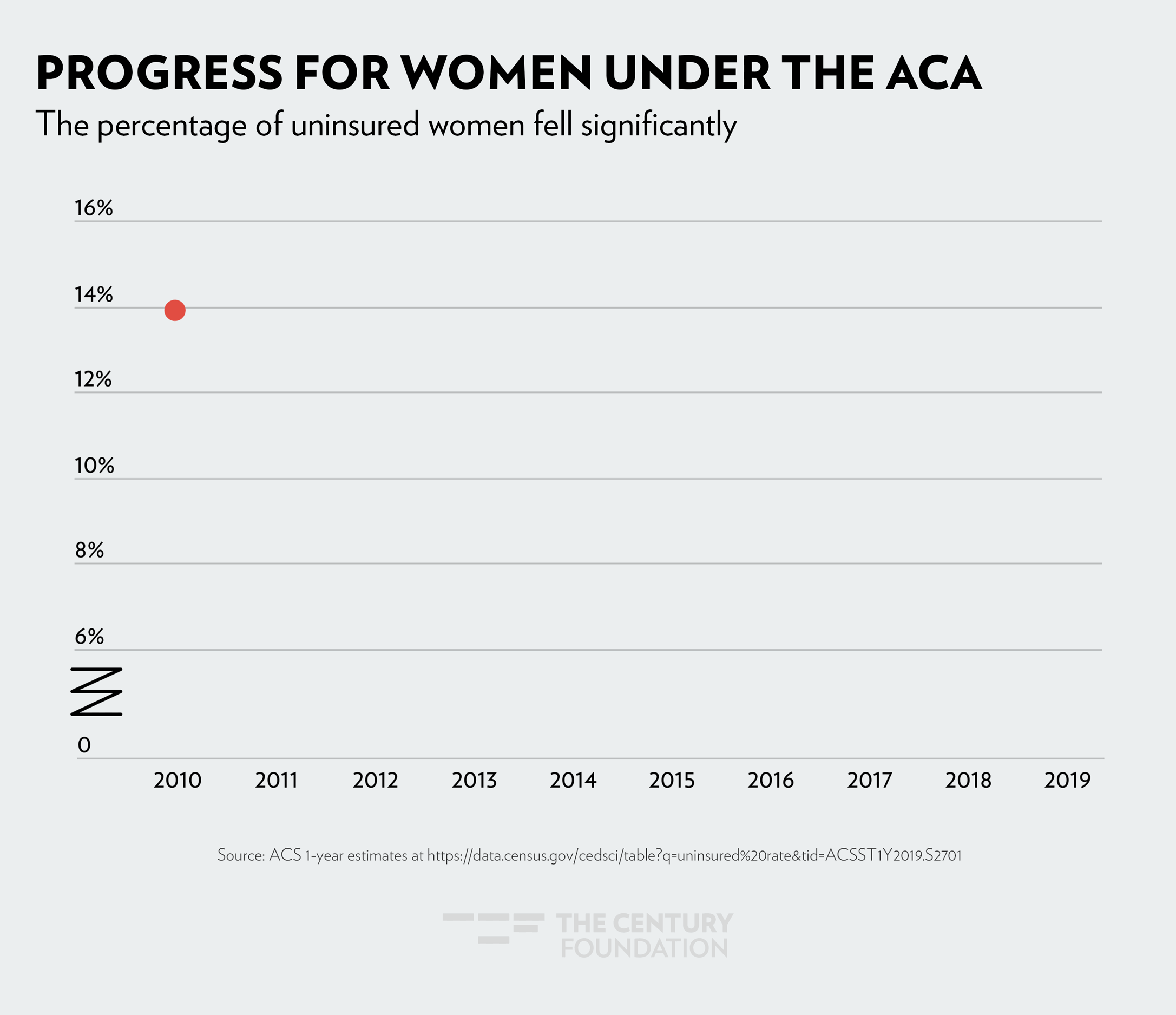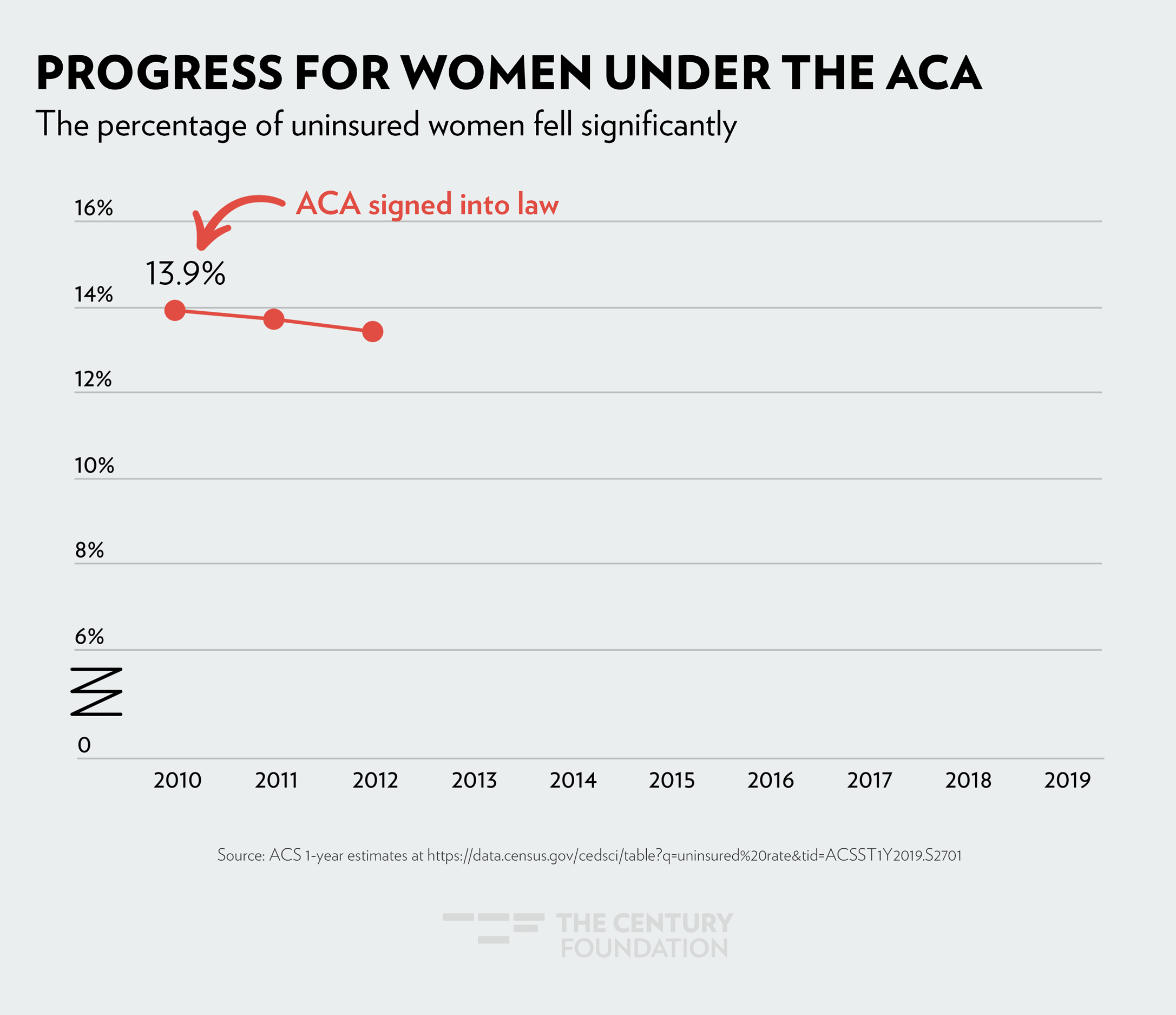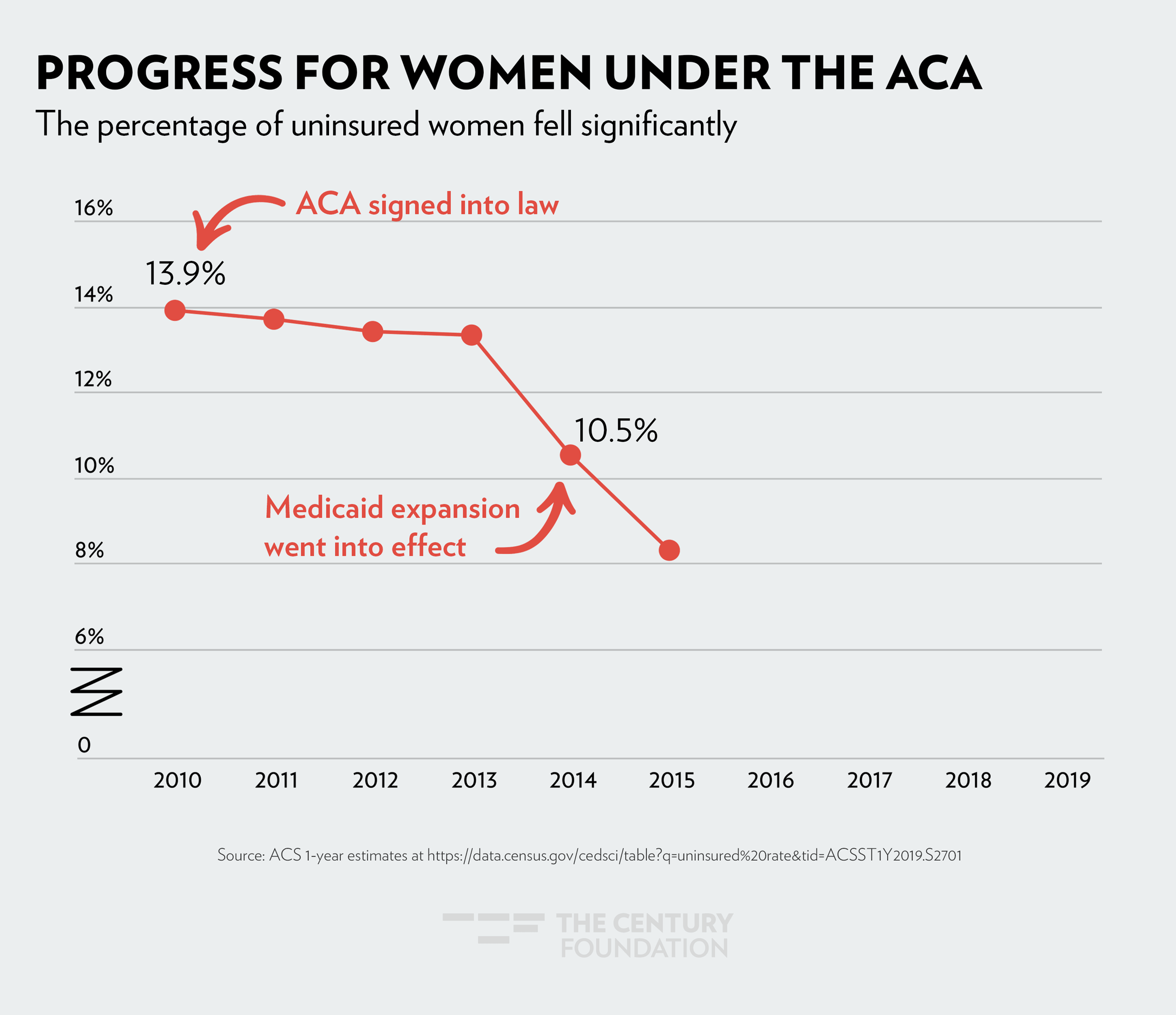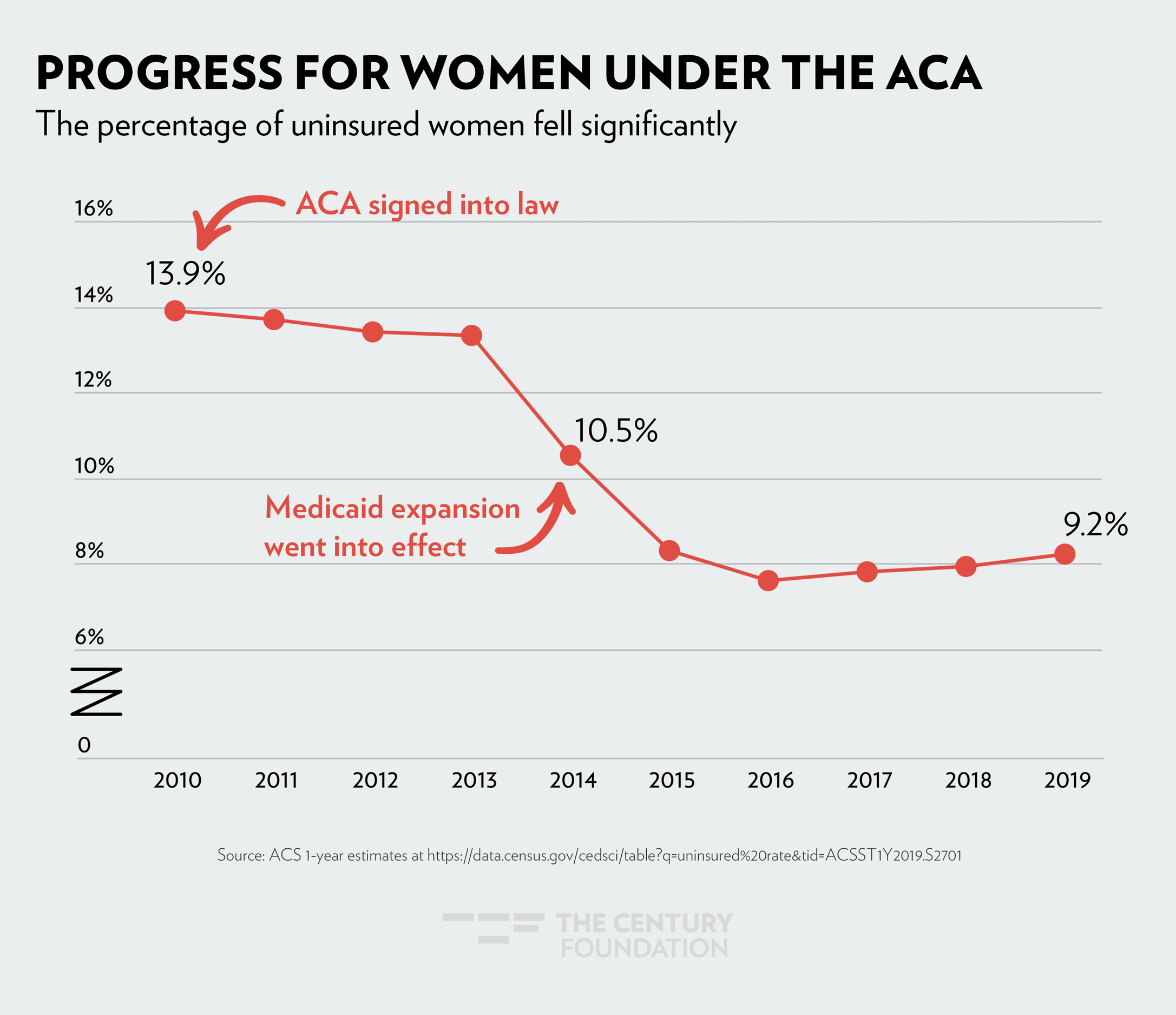
Figure 2
Figure 3
Essential Health Benefits
In addition to efforts to make health coverage more affordable, the ACA required health insurers to cover a standard set of benefits, called “essential health benefits” (EHBs). EHBs are ten broad categories of services that private insurance generally must cover. Some of these benefits drove improvements in health care outcomes, making needed care much more affordable for insured patients.
Many aspects of family planning and maternal health care are covered as EHBs. The National Women’s Law Center estimates that around 62.1 million women in the United States now have insurance that offers contraceptives with no cost-sharing. The ACA’s contraceptive mandate alone saved users an average of approximately $250 a year—savings that add up, as nearly all women use a contraceptive method at some point in their lives. Before the requirement of maternity coverage, pregnant people could have been on the hook for tens of thousands of dollars if their insurance didn’t cover maternity care.
The ACA also requires coverage of preventive services, which has improved access to crucial care. If the U.S. Preventive Services Task Force assigns an A or B rating to any preventative service, insurers are required to cover it without cost-sharing. Well-woman visits, which provide a variety of preventive services, are now required to be covered with no cost-sharing at least once a year. MSM have also benefited from this requirement: insurers are now required to cover pre-exposure prophylaxis (PrEP) drugs, which prevent HIV transmission, without cost-sharing, as well as screening for the disease.
Discrimination Protections
Section 1557 of the ACA prohibits discrimination in health care settings that receive federal funds. The section was the first federal law to prohibit discrimination in health care based on sex. Under the Obama administration, the Department of Health and Human Services (HHS) issued strong regulations prohibiting discrimination based on gender identity and sexual orientation and promoting language access for patients with limited English proficiency. Around 15 percent of LGBTQ Americans surveyed in June 2020 have reported facing discrimination by health providers, and patients with limited English proficiency frequently have worse health outcomes than patients with greater English proficiency.
These protections can be subject to regulatory changes from presidential administrations, however. In 2020, the Trump administration issued final regulations for Section 1557 that would have significantly undermined their benefit to vulnerable patients. While the U.S. Supreme Court ruling in Bostock v. Clayton County (and the resulting HHS guidance)—which held that laws prohibiting discrimination on the basis of sex also apply to sexual orientation and gender identity—prevented some of the more egregious harms, aspects of the regulation reducing protections for interpretation and translation services and permitting blanket religious exemptions for abortion and other necessary medical care were able to go through.
Looking Forward
The ACA has notably improved the health of women, people of color, and LGBTQ people in the United States—and more can be done to build on these gains. Universal coverage is a key component of health equity, but it has yet to be achieved. Closing the Medicaid coverage gap and extending the American Rescue Plan Act tax credits, which subsidize marketplace coverage for middle-income households, will ensure that coverage will be affordable for all patients, regardless of income. These efforts are critical to reducing disparities in coverage: people in the Medicaid coverage gap are disproportionately likely to be people of color: Black and Latino people make up nearly 60 percent of the coverage gap, despite being only around 36 percent of the population in states that have not expanded Medicaid. Similarly, the American Rescue Plan Act made health insurance significantly more affordable, especially for Black people, and its health provisions should be made permanent to maintain these improvements.
In addition to expanding coverage through the ACA, policymakers must work to make that coverage more meaningful, as they did in 2010. Requiring states to permanently extend postpartum Medicaid coverage to one year, for example, is a reform that would go far to address the United States’ maternal mortality crisis. Currently, states are only required to provide coverage under Medicaid for sixty days postpartum, leaving many new mothers without health insurance during a critical period where they are most vulnerable to experiencing maternal mortality and morbidity. Similarly, passing the Black Maternal Health Momnibus Act of 2021 would enact a variety of reforms improving maternal health outcomes, especially for Black women. This package of twelve bills includes improvements such as requiring the Centers for Medicare and Medicaid Services to improve the integration of telehealth into maternal care and establishes a new demonstration project to promote equity and quality in Medicaid maternal care.
These reforms are just a part of moving to an anti-racist health policy approach. Structural racism drives inequities within the health care system, influencing who gets insurance and who does not, as well as driving disparities in outcomes, even among insured patients. Codifying strong implementations of anti-discrimination protections for health care services is another way to ensure that all patients have meaningful access to the health care they need.
Finally, enhancing data collection is another important way to build on the successes of the ACA. While the law has greatly expanded access to health insurance and care, data on the quality of care patients receive are often lacking or unused. This is especially true for LGBTQ Americans: federal data collection efforts are often scant and inconsistent. Surveys by various agencies often do not include questions about sexual orientation or gender identity, and when they do, there is little guidance on how the questions are asked. Without consistent, high-quality data in place, patient needs cannot be understood, much less addressed.
Twelve years after becoming law, the ACA has markedly improved the health care of millions of Americans. Expanding access to coverage across the country—especially for the most vulnerable patients—has brought us closer to achieving health equity, and improving the value of that coverage has ensured that more people are getting the care they need. Building on the ACA’s successes and addressing its areas for improvement will only move the United States further toward a truly equitable health system.
Tags: health care, affordable care act, universal healthcare
The ACA Improved Access to Health Insurance for Marginalized Communities, But More Work Is Needed to Ensure Universal Coverage
The Affordable Care Act (ACA) was signed into law twelve years ago, on March 23, 2010. In the years since, the United States has seen remarkable progress in access to affordable health coverage and health care. Before the law was passed, around 18 percent of the population—more than 46.5 million people—were uninsured. The most recent estimates from mid-2021 put that number now at only 8.9 percent, or about 29.5 million people.
These gains in coverage were concentrated among marginalized groups who were more likely to lack health coverage before the ACA was enacted. Far too many Americans remain uninsured and underinsured, however. This commentary outlines how several provisions of the ACA improved health equity—ensuring that every person has a fair opportunity to be healthy regardless of their social circumstance or identities—for women, LGBTQ people, and people of color. It also describes several ways to build on the successes and structure of the ACA to move further toward universal health coverage, a necessary component of achieving full health equity.
Coverage Affordability
As the name suggests, several components of the Affordable Care Act focused on making health coverage more affordable for consumers who struggled to maintain care due to cost. In this section, we describe how two of these—Medicaid expansion and pre-existing conditions protections—have made health coverage much more affordable for women, LGBTQ people, and people of color.
Medicaid Expansion
Medicaid is a joint state and federal program that provides public health insurance to low-income households. States generally have leeway to set the eligibility and benefit standards for their residents, within broad federal guidelines. The ACA originally sought to require all states to cover every resident up to 138 percent of the federal poverty line (FPL), addressing the patchwork of thresholds that often left childless adults ineligible even at 0 percent of the FPL. Under this expansion, the federal government would pay 90 percent of the costs associated with the newly eligible population. While the requirement to expand Medicaid was eventually found unconstitutional, Medicaid expansion was kept in place as an option for states, and most states and the District of Columbia have expanded Medicaid under the law.
All three groups that this piece focuses on are more likely to have lower incomes. In 2019, women were more than 20 percent more likely than men to have incomes below the poverty line. Similarly, the poverty rate for Black people was more than 2.5 times higher than it was for white people in 2019, and it was more than twice as high for Hispanic people in the same year. Researchers at UCLA estimated in 2019 that LGBTQ people were around 37.5 percent more likely to have incomes below the poverty line as cisgender, heterosexual people. These major disparities in income resulted in Medicaid expansion under the ACA improving all three groups’ access to high quality, affordable coverage.
However, because Medicaid expansion eventually was made voluntary for states rather than a requirement, the efficacy of the provision was reduced. Around 2.2 million people fall into the Medicaid coverage gap—that is, their incomes are too high for their states’ non-expanded Medicaid program, but too low to afford another source of coverage. Eight of the twelve states that have not yet expanded Medicaid are in the South and have disproportionately high Black and Hispanic populations, meaning these states’ decision not to expand raises severe health equity concerns.
Medicaid expansion not only improved access to coverage, but also is associated with improvements in health outcomes. Medicaid coverage of pregnancy-related care is extremely generous, and it is provided with no cost-sharing to the pregnant person. As a result, states that expanded Medicaid have around 1.6 fewer maternal deaths per 100,000 women than states that have not. This is especially crucial to improving health equity, as Black women are roughly three times as likely to die from pregnancy-related causes as white women.
Pre-existing Conditions
In addition to Medicaid expansion, the ACA made several changes to how private health insurance operates. Prior to the law, health insurance companies could charge a higher premium or decline coverage outright based on a person’s medical history. In essence, health coverage was least affordable for the people who needed it most. To address this, the ACA prohibits health insurers from charging people different premiums for any reason beyond age, zip code, and smoking status.
Prohibiting discrimination based on pre-existing conditions has also likely had an outsized impact on women, LGBTQ people, and people of color. All three groups are more likely to have pre-existing conditions that would have precluded them from coverage (or made that coverage far more expensive) before the protections the ACA afforded, and when these identities intersect, it’s even more likely. Many insurers would keep a list of “declinable conditions,” and if a person reported one of these in their medical history, they would be automatically denied coverage.
For example, before the ACA, many health insurers would refuse to cover a pregnant person or would charge a higher premium to a person who had been pregnant before. HIV/AIDS was another condition that was often used to deny or limit coverage before the ACA. Men who have sex with men (MSM) have a one in six chance of contracting HIV in their lifetime, and for Black or Latino MSM, that risk rises to one in two and one in four, respectively. And because of systemic racism, people of color are more likely to have a chronic health condition: 13.8 percent of Black people and 10 percent of Hispanic people have a chronic health condition, compared to only 8.3 percent of white people. Without the protections of the ACA, all of these health conditions could have been used to deny coverage or charge higher premiums.
Coverage Gains under the ACA
The ACA has made health insurance more accessible—particularly for women, people of color, and LGBTQ people. Its provisions, especially Medicaid expansion, have made insurance more affordable and have resulted in substantial gains in health coverage.
The sharpest drop in health coverage was seen in 2014, when Medicaid expansion went into effect. The figures below demonstrate the impact Medicaid expansion has had, by community: Figure 1 shows the decrease in women’s uninsured rate since 2010; Figure 2 shows health coverage by race and ethnicity; and Figure 3 shows how LGBTQ people have gained coverage under the ACA.
Figure 1
Figure 2
Figure 3
Essential Health Benefits
In addition to efforts to make health coverage more affordable, the ACA required health insurers to cover a standard set of benefits, called “essential health benefits” (EHBs). EHBs are ten broad categories of services that private insurance generally must cover.1 Some of these benefits drove improvements in health care outcomes, making needed care much more affordable for insured patients.
Many aspects of family planning and maternal health care are covered as EHBs. The National Women’s Law Center estimates that around 62.1 million women in the United States now have insurance that offers contraceptives with no cost-sharing. The ACA’s contraceptive mandate alone saved users an average of approximately $250 a year—savings that add up, as nearly all women use a contraceptive method at some point in their lives. Before the requirement of maternity coverage, pregnant people could have been on the hook for tens of thousands of dollars if their insurance didn’t cover maternity care.
The ACA also requires coverage of preventive services, which has improved access to crucial care. If the U.S. Preventive Services Task Force assigns an A or B rating to any preventative service, insurers are required to cover it without cost-sharing. Well-woman visits, which provide a variety of preventive services, are now required to be covered with no cost-sharing at least once a year. MSM have also benefited from this requirement: insurers are now required to cover pre-exposure prophylaxis (PrEP) drugs, which prevent HIV transmission, without cost-sharing, as well as screening for the disease.
Sign up for updates.
Discrimination Protections
Section 1557 of the ACA prohibits discrimination in health care settings that receive federal funds. The section was the first federal law to prohibit discrimination in health care based on sex. Under the Obama administration, the Department of Health and Human Services (HHS) issued strong regulations prohibiting discrimination based on gender identity and sexual orientation and promoting language access for patients with limited English proficiency. Around 15 percent of LGBTQ Americans surveyed in June 2020 have reported facing discrimination by health providers, and patients with limited English proficiency frequently have worse health outcomes than patients with greater English proficiency.
These protections can be subject to regulatory changes from presidential administrations, however. In 2020, the Trump administration issued final regulations for Section 1557 that would have significantly undermined their benefit to vulnerable patients. While the U.S. Supreme Court ruling in Bostock v. Clayton County (and the resulting HHS guidance)—which held that laws prohibiting discrimination on the basis of sex also apply to sexual orientation and gender identity—prevented some of the more egregious harms, aspects of the regulation reducing protections for interpretation and translation services and permitting blanket religious exemptions for abortion and other necessary medical care were able to go through.
Looking Forward
The ACA has notably improved the health of women, people of color, and LGBTQ people in the United States—and more can be done to build on these gains. Universal coverage is a key component of health equity, but it has yet to be achieved. Closing the Medicaid coverage gap and extending the American Rescue Plan Act tax credits, which subsidize marketplace coverage for middle-income households, will ensure that coverage will be affordable for all patients, regardless of income. These efforts are critical to reducing disparities in coverage: people in the Medicaid coverage gap are disproportionately likely to be people of color: Black and Latino people make up nearly 60 percent of the coverage gap, despite being only around 36 percent of the population in states that have not expanded Medicaid. Similarly, the American Rescue Plan Act made health insurance significantly more affordable, especially for Black people, and its health provisions should be made permanent to maintain these improvements.
In addition to expanding coverage through the ACA, policymakers must work to make that coverage more meaningful, as they did in 2010. Requiring states to permanently extend postpartum Medicaid coverage to one year, for example, is a reform that would go far to address the United States’ maternal mortality crisis. Currently, states are only required to provide coverage under Medicaid for sixty days postpartum, leaving many new mothers without health insurance during a critical period where they are most vulnerable to experiencing maternal mortality and morbidity. Similarly, passing the Black Maternal Health Momnibus Act of 2021 would enact a variety of reforms improving maternal health outcomes, especially for Black women. This package of twelve bills includes improvements such as requiring the Centers for Medicare and Medicaid Services to improve the integration of telehealth into maternal care and establishes a new demonstration project to promote equity and quality in Medicaid maternal care.
These reforms are just a part of moving to an anti-racist health policy approach. Structural racism drives inequities within the health care system, influencing who gets insurance and who does not, as well as driving disparities in outcomes, even among insured patients. Codifying strong implementations of anti-discrimination protections for health care services is another way to ensure that all patients have meaningful access to the health care they need.
Finally, enhancing data collection is another important way to build on the successes of the ACA. While the law has greatly expanded access to health insurance and care, data on the quality of care patients receive are often lacking or unused. This is especially true for LGBTQ Americans: federal data collection efforts are often scant and inconsistent. Surveys by various agencies often do not include questions about sexual orientation or gender identity, and when they do, there is little guidance on how the questions are asked. Without consistent, high-quality data in place, patient needs cannot be understood, much less addressed.
Twelve years after becoming law, the ACA has markedly improved the health care of millions of Americans. Expanding access to coverage across the country—especially for the most vulnerable patients—has brought us closer to achieving health equity, and improving the value of that coverage has ensured that more people are getting the care they need. Building on the ACA’s successes and addressing its areas for improvement will only move the United States further toward a truly equitable health system.
Notes
Tags: health care, affordable care act, universal healthcare